From Graph to Diet: How Vector Analysis (BIVA) in Follow-up Modifies Nutritional Intervention
The true value of BIA is not in the initial visit, but in monitoring the patient’s trajectory over time
As nutritionists, we know the scene well: the patient returns for a check-up. They step on the scales and the number hasn’t changed. Or, worse, it has dropped too quickly. The frustration (theirs and ours) is palpable. But what really happened during that month? Did the patient lose fat and gain muscle? Are they eating too little and catabolising their precious Body Cell Mass (BCM)? Did they simply drink more before coming to see us? The scales don’t tell us. A scalar BIA analysis (which only gives us FM% and FFM%) gives us a clue, but not the whole story. This is where vector analysis (BIVA), and in particular its use in follow-up, becomes the most powerful clinical weapon at our disposal. If you have already read about the basics of BIVA and the importance of the Phase Angle, now is the time to connect the dots and see how to use these tools to actively guide nutritional therapy. A single BIVA is a snapshot. Vector tracking is the film of the patient’s physiological response to our intervention.
When we take a second measurement, the software of our vector bioimpedance analyser will show us (or allow us to track) the displacement of the patient’s vector on the R-Xc graph. This ‘tracking’ is at the heart of follow-up analysis.
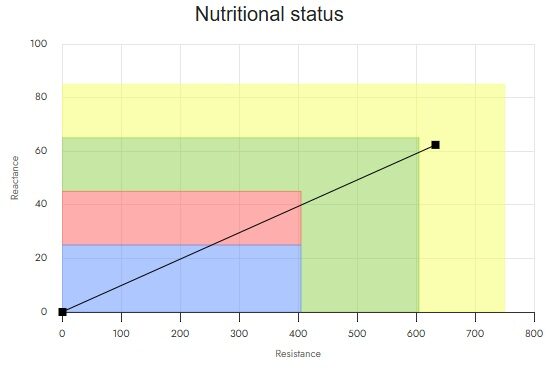
The BIVA graph, as we recall, has two axes:
• Horizontal Axis (Resistance – Rz/H): Inversely proportional to body fluids.
o Shift to the LEFT (↓Rz): The patient has increased fluids (more hydrated, but perhaps also more oedematous).
o Shift to the RIGHT (↑Rz): The patient has lost fluids (less hydrated, less retention, but also potential dehydration).
• Vertical axis (Reactance – Xc/H): Directly proportional to the quantity and quality of Body Cell Mass (BCM).
o UP shift (↑Xc): The patient has built or improved the quality of their cell mass. They have more intact cell membranes. This is almost always a positive sign.
o DOWN shift (↓Xc): The patient has lost cell mass. Their cells are less intact or have decreased in number. This is almost always a negative sign.
Our goal as nutritionists is, almost always, to move the patient’s vector upwards (better BCM) and manage its horizontal shift (fluids) depending on the objective.
Let’s see how this interpretation radically changes our approach.
Case Study 1: The ‘False Plateau’ (Body Recomposition)
• The Patient: Male, 40 years old. He begins a normal-calorie nutrition plan and a strength training protocol. After 6 weeks, the scale reads +0.5 kg. The patient is demotivated: ‘Doctor, I’m struggling for nothing, I’ve gained
weight.’
• BIVA Analysis: The vector has shifted significantly UP (↑Xc) and slightly to the LEFT (↓Rz).
• Interpretation: The patient has not ‘gained weight.’ The increase in reactance tells us that he has built Cellular Mass (BCM). The shift to the left (increase in fluids) is consistent with the increase in muscle glycogen
and intracellular water (ICW) linked to the new lean mass. His Phase Angle has improved.
• Nutritional Action:
1. Reassure the patient: Show them the graph and explain that they are successfully recomposing their body (more engine, less unnecessary ‘bodywork’).
2. Dietary changes: None! Or at most, a slight adjustment in protein or calories to support further growth. Do not cut calories thinking you need to ‘compensate’ for the weight gain.
Case Study 2: ‘Bad’ Weight Loss (Catabolism)
• The Patient: Female, 55 years old, sedentary. She follows a drastic ‘do-it-yourself’ low-calorie diet (e.g. 800 kcal/day). She arrives for her check-up after 4 weeks, proud to have lost 5 kg.
• BIVA Analysis: The vector has shifted to the RIGHT (↑Rz), but more importantly, it has ‘crashed’ DOWN (↓Xc).
• Interpretation: The patient has lost weight, certainly. But the shift to the right tells us that she has lost a lot of fluids (dehydration). The vertical collapse of the Reactance is a red flag: she is catabolising BCM.
She is losing muscle, not just fat. Her Phase Angle has worsened, indicating a deterioration in cellular health.
• Nutritional Action:
1. Immediate Intervention: Explain to the patient that her strategy is harmful. She is losing her body’s “engine”, which will lead to an inevitable plateau and weight regain (yo-yo effect) with interest.
2. Dietary Modification: Immediately increase calories to a sustainable deficit level. Ensure adequate protein intake (e.g., 1.2-1.5 g/kg of ideal weight) to protect BCM. Recommend (if possible) the initiation of minimal
physical activity to stimulate muscle.
Case Study 3: The ‘Ideal’ Weight Loss (Quality)
• The Patient: Male, 50 years old, with obesity and metabolic syndrome. He follows a balanced low-calorie diet and has started walking. At the 8-week check-up, he had lost 4 kg.
• BIVA Analysis: The vector shifted decisively to the RIGHT (↑Rz), but maintained or even slightly increased its height (stable Xc or ↑Xc).
• Interpretation: This is the ‘Holy Grail’ of weight loss. The shift to the right indicates a significant loss of fluids (probably excess extracellular water – ECW linked to inflammation and fat) and fat mass. The fact that
the reactance (BCM) is stable or improved tells us that we have protected 100% of his cell mass. The patient lost only what he needed to lose.
• Nutritional Action:
1. Congratulations: To the patient and to ourselves. The strategy is perfect.
2. Diet Modification: Continue with the plan, possibly recalculating the requirements based on the new weight to maintain the correct deficit. There is no reason to change an approach that is preserving the most important
component of the body.
Vector bioimpedance analysis in follow-up elevates us from ‘diet prescribers’ to true ‘body composition strategists’.
Let’s stop navigating by sight based on weight and start making clinical decisions based on the patient’s actual physiological response. BIVA tracking allows us to correct course in real time, reassure the patient during a false plateau, or intervene abruptly before an incorrect diet causes metabolic damage.
Don’t just use BIA as a formality during the first visit. Use it as your compass during every check-up.
